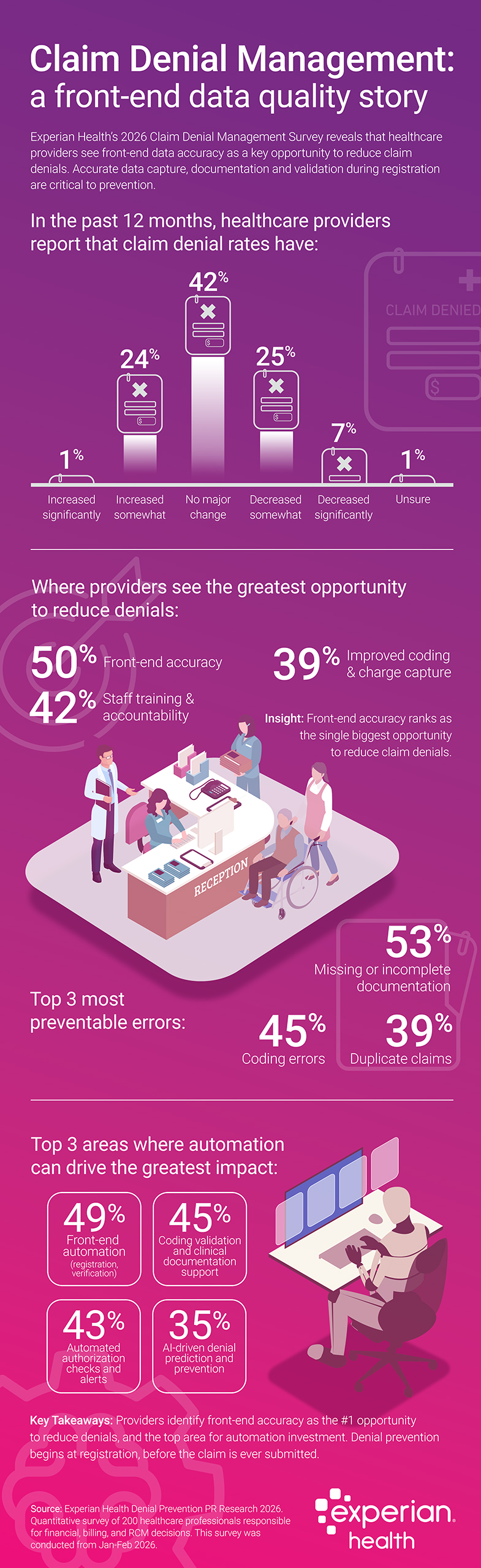
Claim denial charges stay excessive – and in some instances, they’re rising. Experian Well being’s newest Denial Administration survey discovered that over the previous 12 months, 25% of healthcare suppliers reported elevated denial charges, whereas 42% noticed no significant change.
On the identical time, there’s a chance for enchancment. 50% of healthcare organizations establish front-end accuracy as a key alternative to scale back denials. Incomplete documentation, coding, and eligibility errors rank among the many high 5 most preventable causes of claim denials. The implication is evident — many denials stem from preventable data gaps which might be launched earlier than a claim is ever submitted.
The analysis reveals that denial prevention and stronger claims administration start on the entrance finish. When requested the place automation would have the best affect, respondents pointed to front-end and coding validation, automated authorization checks, and AI-pushed denial prediction and prevention.
Denial administration is essentially a front-end data integrity technique. Stopping and decreasing denials begins at registration. Healthcare organizations that shift from denial response to denial prevention – prioritizing correct and full front-end data seize – will see extra sustainable reductions in denials, enhance income predictability and ease administrative burdens throughout the income cycle.
Source link
#frontend #data #problem #claim #denials #Healthcare #Blog




